More than One Health
The modern architecture of global public health was not born organically out of necessity. It was methodically constructed — justified through a succession of engineered crises and manufactured consensus. The true objective was not the eradication of disease, but the quiet transfer of sovereignty: the gradual migration of decision-making from democratically accountable governments to unelected technocratic institutions.
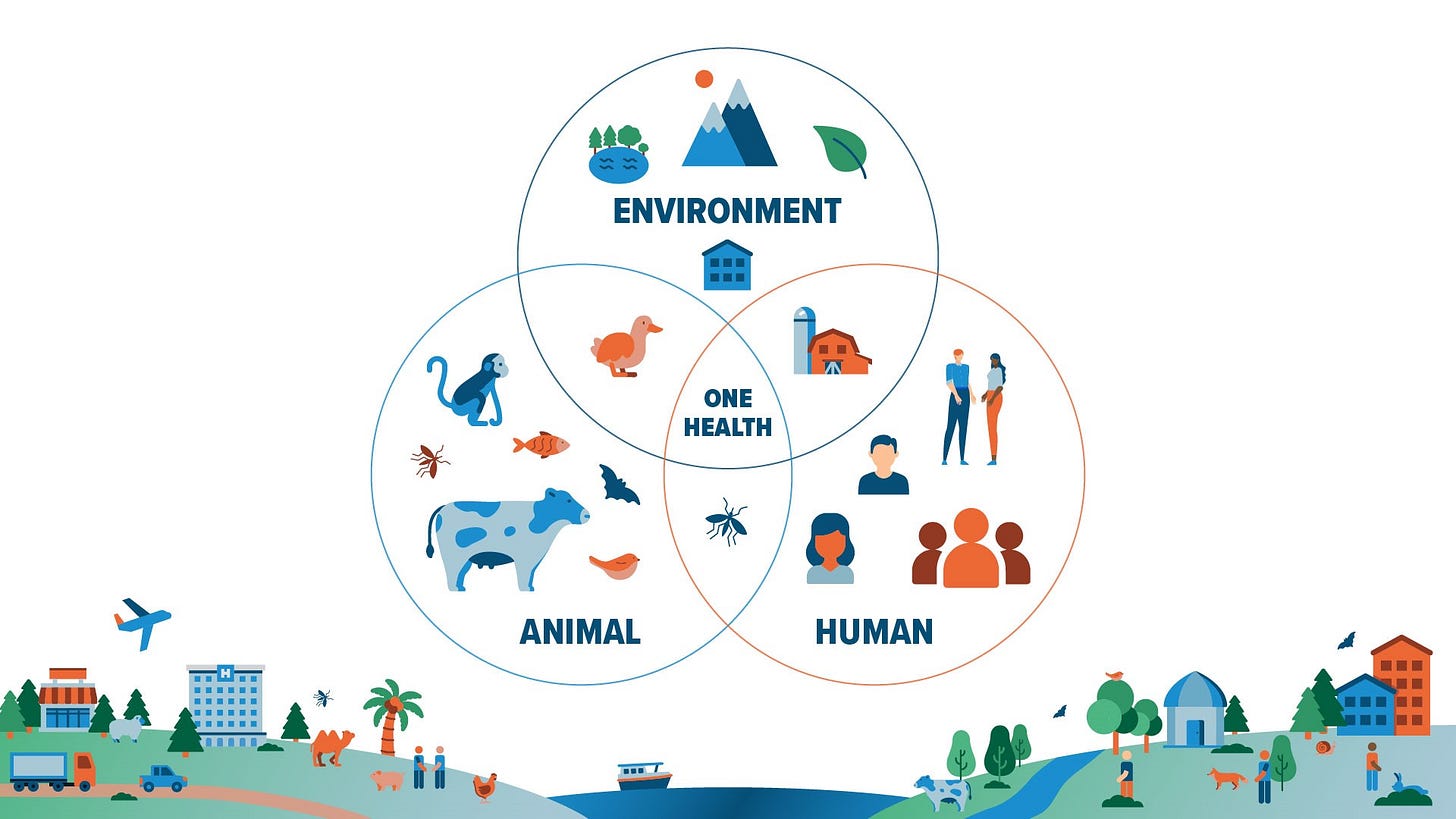
One Health — often marketed as a benign ‘collaborative’ approach — is in truth a framework to control the biosphere in its entirety: humans included. Health policy, environmental policy, agricultural policy, energy policy — all converged into a single, seamless system of surveillance, management, and enforcement.
Johnson's Health Acts
Lyndon B. Johnson’s administration (1963–1969) is best remembered for the Great Society and civil rights reforms, but a quieter revolution unfolded beneath the surface: the federal consolidation of health, environment, and welfare under technocratic management. Driven by the Planning-Programming-Budgeting System1 (PPBS) — an analytic framework imported from military logistics into civilian governance — Johnson’s health legislation systematically integrated public health into a new regime of centralised surveillance and bureaucratic measurement. The Public Health Service Act amendments2 (1965–1968) greatly expanded federal authority over hospitals, patient records, disease reporting, and vaccination programs, bringing health under the same kind of quantitative control as defense and infrastructure.
At the same time, Johnson issued Executive Order 112883 (1966), mandating federal agencies to treat air and water pollution as matters of national health — a fusion of environmental and human welfare management that would later metastasise into broader biosphere governance concepts. Although Johnson left office before signing it himself, his administration laid the groundwork for the National Environmental Policy Act4 (NEPA, 1969), which formalised the doctrine that human prosperity must be evaluated within the holistic management of ecosystems. These moves did not respond to public demand; they were driven by elite advisors and early systems theorists seeking to create a managerial state capable of coordinating life, health, and economy across traditional political boundaries.
By the late 1960s, the conceptual framework was firmly in place: human health, environmental stability, economic growth, and population dynamics were seen as inseparable — and therefore had to be governed together, through technical expertise rather than democratic deliberation. The seeds of One Health were planted long before the term itself would emerge.
By the decade’s end, this managerial vision — originally scoped to domestic health and environment — would begin expanding outward, as global institutions quietly adopted the same systemic governance logic on an international scale.
The Long March
Throughout the 1970s and 1980s, the separation between public health and environmental management steadily eroded, not by popular demand but by elite-driven initiatives in the name of 'sustainability'. The 1968 UNESCO Biosphere Conference5 marked a critical, if underexamined, turning point: for the first time, zoonotic disease was discussed as a global systems management issue, framed within the metaphor of 'Spaceship Earth'6 — a closed ecological system requiring technical stewardship. Shortly thereafter, the Scientific Committee on Problems of the Environment7 (SCOPE) published its first reports (1971, 1973)8, outlining the necessity of integrating human health surveillance with environmental monitoring. By 1974, the UNEP Governing Council (UNEP/GC/24)9 formally expanded the Global Environmental Monitoring System10 (GEMS) to include public health data, embedding human disease surveillance into what was ostensibly an environmental framework.
Simultaneously, high-profile initiatives reinforced the narrative that human health could only be protected through sweeping control of the environment. The World Population Conference11 (1974) linked fertility control to ecological preservation. The Alma Ata Declaration12 (1978) by the WHO promoted 'Health for All'13, stressing that governments must manage determinants like housing, food systems, and environmental quality. And the Brundtland Commission's 'Our Common Future'14 (1987) firmly established the doctrine that human survival depended on comprehensive environmental regulation. These were not public mandates, but elite treaties and declarations, produced by committees far removed from any direct electoral oversight.
Behind the humanitarian language of 'health security' and 'sustainability', a deeper agenda quietly advanced: the construction of a global surveillance and management grid across the biosphere, including its human populations. Organisations like the Rockefeller Foundation quietly funded early prototypes of integrated disease surveillance15, trialling the merger of human, animal, and environmental health into a single governance model. The official justification was always framed in terms of existential risk — zoonotic spillovers, pandemics, ecological collapse — but the function was increasingly obvious to those paying close attention: the incremental centralisation of life itself under expert control, without public consent.
The Acceleration
The Rio Earth Summit16 (1992) marked the public unveiling of a new doctrine: that environmental, economic, and health systems must be globally managed in concert. Agenda 2117 quietly proposed supranational 'coordination mechanisms' for integrated governance, while the WHO's 1992 Our Planet, Our Health18 declaration the same year formally embedded zoonotic disease within the broader mandate of planetary systems management. In parallel, the European Union advanced new legislation19 to harmonise zoonotic disease monitoring across member states20 — an early institutionalisation of human-animal-environment surveillance under the rubric of public health.
Inside scientific and military circles, the same theme was taking shape with sharper edges. Joshua Lederberg's 1992 report, Emerging Infections: Microbial Threats to Health in the United States21, called for a global infectious disease surveillance system, merging human, animal, and environmental monitoring. By 1996, President Clinton's National Science and Technology Council directive (NSTC-7) formally tasked the US Department of Defense with building such a network22, leading to the creation of the Global Emerging Infections Surveillance (GEIS) programme in 199723. While GEIS was justified in terms of force protection, it rapidly became clear that its reach extended far beyond military interests: GEIS laboratories linked into global WHO data-sharing networks, meaning that intelligence gathered for 'force health protection' would flow seamlessly into civilian and international public health infrastructures. Military, public health, and supranational governance were becoming operationally indistinguishable.
By the late 1990s, financial institutions also began quietly preparing instruments to integrate pandemic preparedness into sovereign debt markets and insurance models, setting the stage for future pandemic bonds and 'catastrophe financing' mechanisms. Though largely unnoticed at the time, pandemic governance was already being tied to financial surveillance and risk securitisation — extending control not just over health, but over the economic sovereignty of nations themselves.
By the time the Manhattan Principles24 were finalised at the Rockefeller Center in 2004, the framework was in place. 'One Health' — total integration of human, animal, and environmental health — was no longer a speculative ideal but a rapidly advancing operational doctrine. From the outset, the goal was not flexibility or local resilience. It was harmonisation, standardisation, and enforceable compliance: a surveillance and management regime stretching across the biosphere, under the authority of technocratic institutions largely shielded from public accountability.
Manufacturing Pandemic Governance
The highly dubious H5N1 avian flu scare between 199725 and 2005 served as a vital real-world pilot for the emerging biosecurity governance structure. Although only 17 human cases were recorded during the initial 1997 Hong Kong outbreak26, the unprecedented culling of 1.6 million chickens — originating with Neil Ferguson and the BSE outbreak in the United Kingdom in 199627, and enforced on highly speculative grounds — set a global precedent: that mass livestock destruction, population surveillance, and vaccine stockpiling could be justified not on demonstrated threat, but on projected models. It normalised the doctrine that predictive scenarios, rather than empirical evidence, could dictate sweeping policy interventions — a logic that would later underpin the global response to Covid-19.
At the heart of this shift stood the European Scientific Working Group on Influenza28 (ESWI), founded quietly in 1992 and heavily funded by pharmaceutical interests29. Later in the decade, ESWI members drafted the 1999 WHO Influenza Pandemic Plan, embedding frameworks for mass surveillance, accelerated vaccine approvals, corporate indemnities, and expansive biosecurity interventions into global public health doctrine. Far from acting as a neutral advisory body, ESWI functioned as a strategic bridge between private sector interests and supranational policymaking — systematically institutionalising 'preparedness' doctrines that consolidated authority while creating guaranteed markets for pharmaceutical products.
The pattern tightened with the Pilanesberg Resolution3031 (2001), spearheaded by networks including the IUCN and AHEAD, which pushed for systematic cross-sectoral surveillance of animal and human diseases under a unified, enforceable framework. This shift was not limited to medical management; financial mechanisms soon followed, with early pandemic insurance and securitisation models being quietly trialled by multilateral institutions. By 2004, under the stewardship of figures like William Foege, Steve Osofsky, and William Karesh32 — many of whom would later drive 'Planetary Health'33 and EcoHealth Alliance34 initiatives — the Manhattan Principles were finalised, branding the full convergence as 'One Health'. What H5N1 demonstrated was not the risk of zoonotic spillover itself, but how the invocation of speculative risk could trigger extraordinary regulatory powers — collapsing the boundary between public health management and planetary governance.
The Full Turn to Surveillance Biopolitics
The attacks of 11 September 200135 were a watershed not just for security policy, but for public health governance. The Patriot Act36 (2001) dramatically expanded the federal government's surveillance powers under the justification of counterterrorism, obliterating long-standing constitutional protections. Communications, banking transactions, travel patterns, health records — all became legitimate targets of state scrutiny, often with minimal or no judicial oversight. In parallel, the ECHELON37 revelations confirmed that the Five Eyes38 alliance had long been systematically intercepting communications of European politicians, corporations, and civilians — exposing that mass surveillance was not a contingency but a structural feature of the emerging global order.
Weeks later, the anthrax letter attacks39 — whose perpetrator was never conclusively identified — crystallised the narrative that public health emergencies were national security threats, requiring military-style surveillance and control. In 2002, Congress passed the Public Health Security and Bioterrorism Preparedness and Response Act40, formally merging health infrastructure with national security doctrine. The Act expanded vaccine stockpiling, pathogen surveillance laboratories, and authorised sweeping monitoring of 'critical' sectors under biodefence rationales. The Department of Homeland Security (DHS), itself founded in 2002, would by 2005 release its National Strategy for Pandemic Influenza41 — coordinated jointly with the Department of Health and Human Services (HHS) — effectively blueprinting a global pandemic surveillance and emergency governance system, years before COVID-19.
The shift was definitive: health, environment, finance, mobility, and communication were no longer distinct policy domains. They were reclassified as interconnected security spheres, demanding continuous oversight, pre-emptive regulation, and resilience-building. Public health governance was no longer primarily a medical affair, but a branch of biosecurity logistics — a natural fit with the expanding One Health ideology, and a crucial precursor to the earth systems governance models that would later subsume both biosurveillance and financial resilience under a single cybernetic architecture.
One Health Today
Today, One Health has metastasised far beyond academic white papers and regulatory margins. It has become the dominant framework through which governance of the total human ecosystem42 is now justified — not through democratic consent, but through appeals to 'ethics', 'planetary responsibility', and systemic risk management.
The Pandemic Treaty43 (draft, 2024) proposes legally binding global surveillance, centralised vaccine development and stockpiling, the enforcement of One Health standards, and emergency powers for the WHO — all without national referenda or parliamentary ratification. Simultaneously, the rollout of Central Bank Digital Currencies44 (CBDCs) and Digital ID45 systems, formalised through Sustainable Development Goal 16.946, will integrate individual biometric, medical, and financial data into unified surveillance architectures. Justified under the rubric of 'global health security'47, this infrastructure will operationalise continuous governance of identity, movement, social access, and financial behaviour — in real time.
Most strikingly, the Berlin Principles48 (2019) reframed the very ethical foundations of governance: protecting human health was declared morally inseparable from protecting 'all other life forms'. Under this model, human beings are no longer sovereign political actors but components of a managed biosphere — ethically equivalent to livestock, forests, and migratory species. Surveillance, restriction, and behavioural modification — including through the Social Determinants of Health49 (SDoH) framework — are no longer presented as political infringements, but as moral imperatives for 'biospheric stewardship.'
The pattern is unmistakable: fear of pandemics provided the gateway; technocratic frameworks provided the vehicle; financial instruments secured compliance; and ethics provided the absolution.
Directive Ethics
The aftermath of the 2001 anthrax attacks did more than accelerate biosurveillance and pharmaceutical security; it fundamentally altered the language of governance itself. Under the guise of necessity, a new moral framework was introduced: bioethics50. Initially framed around laboratory safety, informed consent, and bioterrorism defence, this discourse quickly expanded beyond its original scientific bounds, providing a flexible justification for systemic interventions across society.
By the mid-2000s, virtually every major institution — from the WHO to the UN Framework Convention on Climate Change — was issuing declarations of 'ethical responsibility.' In 2009, at the Copenhagen climate summit (COP15), 'climate ethics'51 formally entered the political lexicon — all while Climategate clearly outlined that the science was not quite settled. Protecting the planet was now framed as a moral duty capable of overriding democratic processes and national sovereignty. Ethics panels, compliance frameworks, and advisory boards became institutional fixtures, ensuring that surveillance, mobility restrictions, mass vaccination programmes, and financial penalties could be imposed not as political impositions, but as moral necessities.
This system reached operational maturity during the Covid-19 crisis. Every intrusive measure, from lockdowns to forced medical interventions, was justified not merely as policy but as an ethical imperative to protect collective health. Doctors who questioned official narratives or vaccine mandates were not simply dissenting; they were cast as unethical actors, stripped of licences and livelihoods. Meanwhile, environmental governance followed the same pattern: personal behaviour, financial transactions, and even private energy use were recast as subjects of ethical monitoring and sanction.
Within this framework, ethics — far from serving as a restraint on power — became a sophisticated instrument of systemic enforcement: a moral shield for technocratic governance, operating beyond public vote, immune to judicial challenge, and weaponised to reframe dissent as moral deviance rather than political disagreement.
Evolution of Pandemic Planning
The notion of pandemic planning did not emerge organically in response to public health needs. It was constructed, iterated, and refined over decades — always closely linked to broader ambitions of surveillance, behavioural control, and the merging of health governance with environmental and financial management.
The 1976 Swine Flu52 scare at Fort Dix — involving a handful of US army recruits and no sustained human-to-human transmission — triggered the first mass vaccination campaign against an alleged pandemic threat53. It failed disastrously: the rushed vaccine caused hundreds of cases of Guillain-Barré syndrome, outstripping the disease itself in harm. Yet this episode coincided suspiciously with the 1976 Rougemont Conference54 — a pharmaceutical industry summit, where digital surveillance, universal vaccination, and 'interdependence management' were central themes. Notably, the opening and closing remarks were delivered by Walter Dowdle55, Deputy Director of the CDC, signalling direct institutional alignment. Two years later, CDC Director William Foege signed off on the United States' first formal pandemic response framework56 — a plan obsessed with rapid vaccine deployment, 'community mitigation' (early lockdown theory), and cross-sectoral emergency coordination.
Simultaneously, the Alma-Ata Declaration on Primary Health Care57 (1978) laid the ideological foundations for supranational health governance: universal care would be delivered not through direct democratic accountability, but through trisectoral networks — harmonising public, private, and civil society actors under international guidance. This model anticipated the subsidiarity principles later embedded into Agenda 21 and the broader Third Way political framework: devolution where politically useful, centralisation where strategically necessary — but with central planners always able to override local decisions top-down.
By 1993, the European Scientific Working Group on Influenza (ESWI) — heavily funded by pharmaceutical corporations — had begun drafting the first truly international pandemic influenza strategies. Their 1999 collaboration with the WHO produced the official WHO Influenza Pandemic Plan, while the anthrax scare after 9/11 pivoted pandemic planning decisively into the national security apparatus, militarising what had previously been a civilian public health domain.
Yet the true blueprint for Covid-19 was finalised quietly in 2006. The World Bank/WHO document, Responding to Avian Influenza and Pandemics: A Framework for Global Preparedness58, openly called for the construction of permanent global surveillance grids, pre-negotiated vaccine and antiviral contracts, rapid livestock culling protocols, restrictions on civil liberties, and the full operational integration of health, agriculture, security, and finance sectors. Crucially, it proposed the development of financial instruments — such as emergency disbursement funds, bond-based pandemic insurance, and private sector 'preparedness' contracts — to tie pandemic governance directly into the architecture of sovereign debt and risk securitisation. This fusion would later be formalised through initiatives like the World Bank Pandemic Emergency Financing Facility59 (PEF, 2017).
Today, with the WHO's proposed Pandemic Treaty (2025), the system is being codified into international law: binding obligations for nations to submit to centralised pandemic governance, enforced through 'One Health' integration, financial conditionalities, and permanent biosurveillance infrastructure. What began as speculative crisis planning is now intended to be absolute — a standing system of managed emergency governance, operating continuously across health, economy, environment, and society.
From Health to Biosphere Sovereignty
Today, One Health is no longer merely a health initiative. It is the health pillar of a much larger governance project: the consolidation of control over the total biosphere, including humanity, under a cybernetic model of planetary management.
Through Agenda 21, the Biosphere Conference of 1968, the GEMS environmental surveillance systems, and the emergence of Earth Systems Governance60 frameworks post-2009, elites constructed a vision in which the planet, its climate, its species — and increasingly, human thought and behaviour — must be treated as interconnected components of a single, monitorable, governable system. Within this model, 'health' was never primarily about pathogens; it was a vector for rationalising the permanent capture of human populations into the same management apparatus as forests, wetlands, livestock, and migratory birds.
The One Health Berlin Principles61 (2019) formalised this transformation: human health, animal health, and environmental health are now declared morally equivalent. The survival of a human being is treated as no more ethically privileged than that of any other species. Under this doctrine, pandemic interventions are no longer about protecting individual rights or freedoms, but about mitigating systemic risks to the broader planetary system. The moral pivot — elevating the collective biosphere over human autonomy — has been largely invisible to the public, who are still invited to believe that health restrictions serve their direct personal welfare.
But the redefinition of health was only the beginning.
The New Planetary Governance Model
At the same time, the ethical frameworks developed after 9/11 — under the banners of bioethics, climate ethics, AI ethics62, planetary ethics63, and neuroethics64 — steadily ceased to function as defences of human dignity65. Instead, they evolved into flexible instruments for systemic enforcement. During Covid-19, this shift was made explicit: ethical codes were weaponised to silence dissent, compel medical conformity, and redefine informed consent as conditional upon perceived collective benefit. Doctors and scientists were not punished for factual error, but for ethical noncompliance. Ethics, surveillance, emergency law, and public health were fused into a single mechanism of administrative control — enforced not by political persuasion, but by moral decree.
This fusion accelerated through initiatives like the IUCN-supported AHEAD programme66, which merged wildlife conservation with human health surveillance across Africa, prefiguring the operational rollout of One Health principles. By the mid-2010s, the Planetary Health movement — involving figures like Steve Osofsky67, a co-author of the Manhattan Principles — extended the paradigm further: human civilisation itself was reframed as a patient requiring planetary-scale governance interventions. During the Covid-19 crisis, the Lancet Covid-19 Commission68 made the trajectory unmistakable: among its first six stakeholders (inclusive of Jeffrey Sachs), not a single frontline health professional was included. Instead, the group was dominated by specialists in sustainable development, signalling that pandemic governance had been fully absorbed into the machinery of supranational management under the Sustainable Development Goals69.
This is the culmination of a far longer arc: from early systems theory (Bogdanov’s Tektology), through mid-century cybernetic environmentalism (UNESCO, IIASA, Earthwatch), to the modern cybernetic management of the human ecosystem. Pandemic planning, One Health surveillance, climate modelling, and behavioural modification initiatives all reveal the same underlying architecture: predictive modelling, harmonised data capture, and the pre-emptive reordering of societies through global governance standards — operating permanently above democratic consent.
Financial securitisation mechanisms such as the World Bank’s 2017 Pandemic Emergency Financing Facility (PEF) tied future outbreak responses to private financial instruments — embedding pandemic ‘emergencies’ into speculative markets long before Covid-19 appeared. Meanwhile, surveillance infrastructures like GEIS, initially rationalised for US military biosecurity, were quietly networked into WHO global data-sharing systems — ensuring that information flows served a converged planetary governance apparatus, not national interests.
What confronts us now is not a failure of public health policy. It is the mature realisation of a technocratic project that has always viewed humanity not as citizens with inalienable rights, but as one manageable variable within a planetary operating system — to be monitored, optimised, vaccinated, culled if necessary, and governed indefinitely within a boundary70 through supranational instruments claiming ethical necessity.
The price of freedom is eternal vigilance. But in a world where even the concept of ethics has been reprogrammed to privilege systemic stability over human liberty, vigilance alone will not suffice. Only a clear recognition of the architecture being constructed — and a relentless refusal to surrender sovereignty or truth — offers any meaningful defence.
The Pandemic Treaty’s final draft71 (2025) does not merely create a framework for future emergencies. It cements a standing global governance infrastructure: embedding rapid response hubs, global genomic surveillance networks (such as the International Pathogen Surveillance Network72, IPSN), and contractual frameworks enforcing equitable access to medical countermeasures — regardless of national sovereignty. Preparedness hubs will integrate into WHO-coordinated "One Health" intelligence systems, while Sustainable Development Goal platforms like the SDG 3 Global Action Plan Accelerator73 and the emerging SDG Financing Labs74 will tie compliance to financial conditionalities and sovereign debt instruments. Pandemic response will no longer be an ad hoc process triggered by crises; it will be a continuous operational function of a planetary management system. Governance will no longer flow through electoral accountability but through permanent administrative command — treating the regulation of human life not as an emergency exception, but as the standing operating logic of the global system — while a handful of connected insiders cash out75.
























![WHO Pandemic Agreement [April, 2024]](https://substackcdn.com/image/fetch/$s_!HHbL!,w_140,h_140,c_fill,f_auto,q_auto:good,fl_progressive:steep,g_auto/https%3A%2F%2Fsubstack-post-media.s3.amazonaws.com%2Fpublic%2Fimages%2Fb69c8066-0498-4924-af63-1344abb2ec85_1206x612.png)


























Thanks for the history but I object to your characterization of LBJ. That evil bastard was best known for running an organized crime syndicate in TX that made him an optimal choice to serve as an accomplice in the assassination of JFK and the coverup autopsy. LBJ and fellow demon McNamara conspired to murder thousands in the contrived war in Vietnam and surrounding countries. LBJ’s socialist program were intended to create a culture of failure and dependency that would have, “niggers voting democrat for generations”. And most exemplary, LBJ was having an affair with an Israeli spy during the terrorist attack on the Liberty. Both Johnson and McNamara intervened to turn back rescue air support saying something like, "I don't care if sailors die to protect our best ally...”
Oh, and he shared Fauci’s fetish for torturing beagles.
LBJ should have been hung a hundred times.